|
Visual analog scale qualitative asks patients to mark their current pain level along a continuum of “good day,” “average day,” or “bad day.” The VAS is exactly 10-cm long with “good day” on the extreme left and “bad day” on the extreme right of the line. It is an 11-point scale for patient self-reporting of pain intensity: 0 being no pain, 1 to 3 mild pain, 4 to 6 moderate, and 7 to 10 indicating severe pain. Numeric rating scale is the standard pain assessment tool at Geisinger. This was a prospective, survey study that collected data using the Pain Assessment questionnaire that asked participants to rate their pain on both the VAS and the NRS and state their preference for scales ( Figure 1). There are known discrepancies between NRS and VRS. Verbal rating scales (VRSs) are ordinal scale with descriptors such as none, mild, moderate, and severe which the patient chooses as a category that fits their pain intensity. A VAS uses either a horizontal or vertical line without numbers on which the patient places a mark between the 2 anchors which they feel best describes their pain intensity. 6, 22, 23 The most commonly used unidimensional pain scales are NRSs also known as a numeric pain intensity scale. Anchors though are subjective and are gauged by experience and can shift with ongoing patient experiences of pain. 5, 6 Unlike multidimensional symptom assessment scales such as Edmonton Symptom Assessment Scale and the Brief Pain Inventory, unidimensional scales are quick and easy to use, provide rapid feedback about the effectiveness of interventions and are valid and reliable measures of pain intensity. Various unidimensional numeric rating scales (NRSs) and visual analog scales (VASs) are commonly used to assess pain severity. The minimum clinically important difference at the 1 and 4-week follow-up corresponded to a change of 2.2 and 1.5 points, respectively.Ĭlinicians can be confident that a 2-point change on the NPRS represents clinically meaningful change that exceeds the bounds of measurement error.All subjects Allied Health Cardiology & Cardiovascular Medicine Dentistry Emergency Medicine & Critical Care Endocrinology & Metabolism Environmental Science General Medicine Geriatrics Infectious Diseases Medico-legal Neurology Nursing Nutrition Obstetrics & Gynecology Oncology Orthopaedics & Sports Medicine Otolaryngology Palliative Medicine & Chronic Care Pediatrics Pharmacology & Toxicology Psychiatry & Psychology Public Health Pulmonary & Respiratory Medicine Radiology Research Methods & Evaluation Rheumatology Surgery Tropical Medicine Veterinary Medicine Cell Biology Clinical Biochemistry Environmental Science Life Sciences Neuroscience Pharmacology & Toxicology Biomedical Engineering Engineering & Computing Environmental Engineering Materials Science Anthropology & Archaeology Communication & Media Studies Criminology & Criminal Justice Cultural Studies Economics & Development Education Environmental Studies Ethnic Studies Family Studies Gender Studies Geography Gerontology & Aging Group Studies History Information Science Interpersonal Violence Language & Linguistics Law Management & Organization Studies Marketing & Hospitality Music Peace Studies & Conflict Resolution Philosophy Politics & International Relations Psychoanalysis Psychology & Counseling Public Administration Regional Studies Religion Research Methods & Evaluation Science & Society Studies Social Work & Social Policy Sociology Special Education Urban Studies & Planning BROWSE JOURNALS The standard error of measure was equal to 1.02, corresponding to a minimum detectable change of 2 points. The majority of patients had clinically meaningful improvement after both 1 and 4 weeks of rehabilitation. Change in the NPRS from baseline to the 1 and 4-week follow-up was compared to the average of the patient and therapist's perceived improvement using the 15-point Global Rating of Change scale. To examine the responsiveness characteristics of the numerical pain rating scale (NPRS) in patients with LBP using a variety of methods.Īlthough several studies have assessed the reliability and validity of the NPRS, few studies have characterized its responsiveness in patients with LBP.ĭetermination of change on the NPRS during 1 and 4 weeks was examined by calculating mean change, standardized effect size, Guyatt Responsiveness Index, area under a receiver operating characteristic curve, minimum clinically important difference, and minimum detectable change. 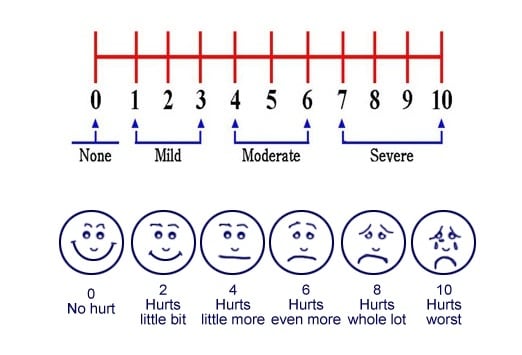
Cohort study of patients with low back pain (LBP) receiving physical therapy.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
